Following the recent events regarding the detention of the former Deputy Minister of Health and ten doctors in the case of fraud with the transplantation system in Ukraine, society is concerned and interested in an honest review of the functioning of this important medical industry. In order to understand the real situation, we turned to a prominent figure in this field, Vasyl Strilka, who is respectfully called the “father” of transplantation in Ukraine.
Back in 2020, when we wrote about the first bone marrow transplant in Ukraine to a child from an unrelated donor, the arrows pointed to Strelka — as the person who powerfully intervened to make this legally possible. Mr. Vasyl now heads the Directorate of High-Tech Medical Care and Innovations at the Ministry of Health.
Where do organs for transplant come from?
"Transplantation is impossible if there is no donor organ," Vasyl Strelka begins. That is, there must be a donor who has been diagnosed as brain dead but whose heart is still beating.
The brain can die due to various reasons. For example, a traffic accident. Or a stroke. According to foreign scientific data, Vasyl adds, about 50% of those who die from a stroke go through the stage of brain death.
In Ukraine, 130,000 Ukrainians have a stroke every year, and over 25,000 of them die. And the numbers are growing.
Brain death is diagnosed in resuscitation and intensive care units. And this is where, says Vasyl, the main problem of the system lies. After all, until a council of doctors gathers and confirms this diagnosis, there can be no question of a person who is actually already dead becoming an organ donor for other living people.
According to the order of the Ministry of Health, which was copied from European and American ones, the diagnosis of brain death must be made for all patients who have three points on the Glasgow coma scale. Even if it is an old grandfather. But in practice, this is not the case.
"I graduated from Bogomolets Medical University in 2012. During my entire education, I was never told anything about brain death, its diagnosis, that such a diagnosis exists. And tens of thousands of such doctors have been graduated. They work. When something comes to your mind that you haven't done before, you think: do I need it? In May 2019, WHO representatives, who were key at that time in transplantation, came to us. I ask one, a Spaniard: "Tell me what you do so that your doctors diagnose brain death?" He didn't understand the question: "You mean? It's their duty." They don't understand our problem. Ours is in the intensive care units," Strelka emphasizes.
He recalls that in 2019 there were practically 0 such diagnoses, only in Zaporizhia region did something happen, one or two people became organ donors there a year. They removed kidneys for transplantation, performed several posthumous kidney transplants throughout Ukraine.
And five years later, few brain death diagnoses are performed in the country. Because, in addition to a directive, there must also be a desire on the part of doctors and the equipment for this.
One doctor said off-record that sometimes, in order for a district hospital to diagnose brain death, a team of specialists from the transplantation center would travel there with their equipment: an ultrasound, a gas analyzer, and so on.
It is important that these are not transplantologists, but an anesthesiologist or neurologist, for example.
Strelka confirms that such a problem exists. Moreover, equipment for such diagnostics should already be in intensive care units and intensive care units, he adds. For example, the same blood gas analyzer to treat patients who end up there.
There is also a corresponding order from the Ministry of Health stating that all this equipment must be there and, if necessary, used to diagnose brain death.
"Is it everywhere? It varies. I would like to be treated in the department where brain death is diagnosed or transplants are performed. Because in that case my chances of survival are higher, because the doctors there are more qualified. They not only have the equipment, but they also use it," explains Vasyl Strilka.
All intensive care units should be able to routinely diagnose brain death themselves. But the reality is not like that. It is often difficult for district hospitals to get started — due to fear and ignorance, he adds: “So it is normal and good to have someone to help get started.”.
And here we come to an interesting and ethically controversial decision by the Ministry of Health in medical circles - agreements on cooperation between hospitals that are transplantation centers and hospitals that are potential bases for removal, that is, where there is an intensive care unit and the ability to diagnose brain death.
Whoever is more active will receive more organs
In order for a transplant center to perform a transplant, save its patient, and receive good money from the state for it, it needs organs.
They can only appear when the intensive care unit diagnoses brain death. Of course, only a fraction of them will be suitable for donation, but it is not 0.
Therefore, the Ministry of Health made it so that transplant centers would be interested in training local hospitals. To this end, cooperation agreements were envisaged in 2021, since transplantation is “a team effort that usually involves several hospitals; the Ministry of Health has written rules to stimulate interaction and cooperation between hospitals.”.
If a transplant center enters into an agreement with a local hospital, trains it, perhaps even shares equipment, it gets priority rights to the organs that become available there as a result of the death of patients.
In off-the-record conversations, doctors involved in transplantation explained that, in particular, this is how the imbalance appeared across the country: some transplantation centers quickly toured many hospitals, signed contracts with them, and now receive the lion's share of organs. It's a kind of principle: whoever jumped in first gets the shoes.
Many agreements were signed, in particular, by the Shalimov Institute, the Heart Institute, and the First Territorial Medical Association of Lviv. According to statistics from previous years, they are the leaders in the number of organ transplants.
What is the solution to the problem and the ethical dilemma here at the same time? The point is that in Ukraine there is and there is not a single waiting list for organs.

Each transplantation center has its own list, already integrated into the general electronic system YEDIST, which we will talk about later.
A patient from a center with many contracts has a higher chance of receiving an organ on time, while another may die before they can receive it. This puts patients with the same indications for transplantation in unequal conditions.
On the one hand, such rules push the system to develop. On the other hand, it is not the patient's fault that his center did not sign many contracts. There were doctors who did not believe that their patients from less agile centers would survive to receive transplants.
Vasyl Strilka replies that it is not a matter of faith, but of the work of doctors with other hospitals. In addition, the system gives first priority to emergency patients who may die without a transplant in a matter of days, outside of all contracts, searching for donors for such people throughout the country.
"In 2018, we had four or five transplant centers that performed only family kidney and liver transplants, and in Zaporizhia, we performed a couple of kidney transplants from a deceased donor. That is, we had people who performed transplants. But they were not active, while they said that they wanted to save people. The Verkhovna Rada adopted a law that gave impetus to the system. And the rules that you have to go to hospitals are an order of the Ministry of Health. We told them about transplantation, the stories of patients who need transplants. These are a couple of thousand people. Because there is no other way to develop the system in an adequate period of time.".
He adds that those transplant centers that work harder, travel to hospitals, give them advice, and as a result transplant more organs. That's why there is a skew, with some performing 100 transplants a year, while others perform two to five: "We see that cooperation between transplant centers and hospitals increases the level of donation.".
He also says that one hospital can now have several agreements with transplant centers. At least with all of them.
Last year, transplants were performed in 26 centers. In total, about 40 centers signed contracts with the National Health Insurance Fund for this purpose.
“There are 12 hospitals that have a stroke center, contracts with the National Health Insurance Fund for transplantation, but did not perform transplants in 2023,” says Strelka. And he adds: if they continue like this, the state will not conclude contracts for transplants for them in 2025.
Instead, those centers that perform transplants are becoming more professional, and it is better for patients to go there, because the chances of receiving a donor organ are higher.
Regarding centers that do not have as many transplants and contracts, Mr. Vasyl says this: in Ukraine there are district hospitals and stroke centers where routine brain death diagnostics have not yet been implemented. You can send your specialists there, sign contracts, and increase transplants.
After all, the Ukrainian system currently covers about 10% of the real need, Strelka points out. And he compares Ukraine with other leading countries in the number of transplants. In the world, this indicator is calculated by the number of transplants per million population. In 2023, Ukraine conducted:
- 61 heart transplants: if we were at the level of Croatia, we would have transplanted 440 hearts;
- 4 lung transplants: if compared to Austria, we should have 505 such transplants;
- 243 kidneys: if compared to the leader, Spain, there should be 2,500 kidney transplants per year.
Currently, there are 3.6 posthumous donors per million population in Ukraine. If you don't count the two or three donors per year who were in Zaporizhia, there were 0 in the country. But Spain has an indicator of more than 40, the USA - more than 40. The average indicator in Europe is 25-40. That is, the Ukrainian system can be increased 10 times, Vasyl argues.
How the algorithm for diagnosing brain death and authorizing organ removal works
Let's move on to another important component of the system - the operation of the transplantation algorithm itself.
When a patient in intensive care has a score of three on the Glasgow Coma Scale, a panel of doctors convenes and diagnoses brain death.
According to Strelka, it's a simple procedure, all the necessary skills were taught at the medical university, they just didn't explain there was such a diagnosis.
For example, you need to check your reflexes, do an apnea test (temporary cessation of breathing), electroencephalography (shows whether there is electrical activity in the brain), and so on.
Vasyl Strilka says that such diagnostics cannot be wrong: "If the study shows that there is no blood flow in the brain, then it is not there. Each doctor checks his own, goes through the checklist determined by the Ministry of Health.".
If the hospital has a cooperation agreement with a transplant center, it can help with diagnostics. For example, send its intensive care specialists, but not transplantologists, provide remote consultation, view online tests and indicators, and advise on adjusting medications somewhere so that the heart does not stop, because then there will be no transplant.
Brain death is diagnosed without reference to transplantation, Strelka emphasizes. After all, studies say: if this diagnosis is tied to transplants, the level of donation becomes small. They say, then doctors can decide by eye: "Maybe this person will be a donor? No," and not even conduct a diagnosis.
After a panel of doctors has declared brain death, doctors check whether the deceased person has any contraindications to donation, such as infectious diseases.
If there are contraindications, according to the order of the Ministry of Health, life support should be stopped. That is, the artificial lung ventilation device should be turned off.
"This is also about human dignity. Because we were told about cases when a stroke was treated in the intensive care unit, the person was already brain dead, not officially diagnosed, and the relatives of the deceased were sent to the pharmacy every day to buy thousands of hryvnias worth of medicine. This should not happen. No one has ever been resurrected after brain death," says Strelka.
And he adds that after a diagnosis of brain death, a person is considered dead according to the law. After all, biological death is irreversible.
Reference. Article 52. Determination of irreversible death of a person and termination of active measures to support the patient's life. Medical workers are obliged to provide full medical care to a patient in an emergency condition. Active measures to support the patient's life are terminated if the person's condition is determined as irreversible death. The moment of irreversible death of a person is the moment of his brain death or his biological death.
If no contraindications are found in a person after the diagnosis of brain death, he is considered a potential donor. At this stage, transplant coordinators of the hospital where the donor is located, or the Ukrainian Transplant Coordination Center, are involved. It is responsible for coordinating the entire system.
If a donor appears, the transplant coordinator of the hospital where the donor is located communicates with the family about consent to organ removal, organizes all necessary tests and enters data into the Unified Transplant Coordination System. The transplant coordinator of the Ukrainian Transplant Coordination Center provides support for the distribution process through the Unified Transplant Coordination System according to the rules of the Ministry of Health.
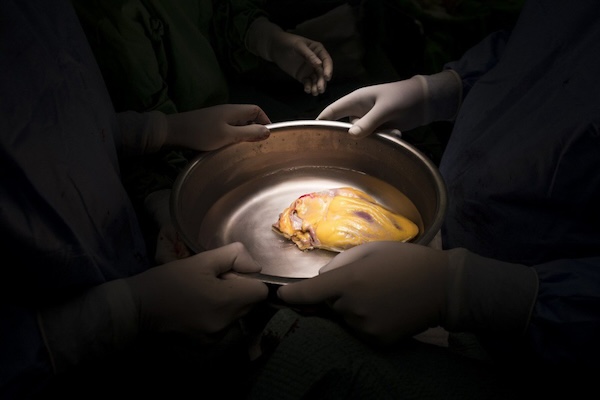
If the relatives have given their consent to the removal of organs, the donor undergoes additional examinations, and only then does an automated system use an algorithm to select potential recipients of the organs that the relatives have agreed to donate. For example, they may allow the removal of the liver and kidneys, but not the heart.
How the system chooses who gets a particular organ: the transplant waiting list
First, the algorithm searches for patients across Ukraine who have an emergency transplant status. That is, if these people do not have an organ for transplantation in the coming days, they will die. No agreements between hospitals matter here.
If there is such a person and they are basically compatible in terms of blood type and anthropometric data (a 50-year-old kidney will not work for a 6-year-old child), the system first offers the organ to them.
The transplant coordinator of the transplant center checks what is happening with her now and informs the Ukrainian Transplant Coordination Center about it. Because yesterday a person could have been alive, today, unfortunately, they are no longer.
Then additional tests. For example, cross-match: the blood of the donor and the organ recipient is checked for compatibility.
If everything is OK and the transplant doctors decide to operate, they plan the transplant. If there is no emergency recipient, that is, a person who urgently needs a donor organ, or something does not fit, the system searches further. It checks whether the retrieval base has a cooperation agreement with a transplantation center.
If it has, it first searches for organ recipients there to see if there are any matches. If the hospital has several contracts with transplant centers, it searches several waiting lists at once.
Can one person be on the waiting list at multiple transplant centers to increase their chances of a transplant?
Strelka explains that no: "If a person needs a transplant, they are very sick. For example, their heart is not working properly. Someone has to take care of such a person. If they were waiting in line at three centers, we wouldn't be able to find the last one.".
If a hospital does not have an agreement with any transplant center, the system searches the entire country at once.
When there are several people who are potentially suitable for a particular organ, the system checks which of them has been in the queue the longest, who has given consent during their lifetime to have their organs removed in the event of their death.
"This is also taken into account. I gave my consent during my lifetime, and someone didn't. All other criteria are the same for us. So it's more fair to give the organ to me, because I was ready to give mine to someone," explains Strelka.
And so a waiting list is formed of those who are basically suitable for an organ that has not yet been removed, but has already received consent from relatives.
Then the doctors come on stage. The center that is higher on the list can agree to take the organ or refuse it, and that's how it happens around the world.
"In the US, every organ, even one that some people think is not very good, will be offered to all transplant centers until the last one refuses," says Strelka. "Colleagues from the US told me about a lung transplant case. All the centers on the list began to refuse them because the donor had partial pneumonia. While the centers were refusing, three days passed, the doctors who were supporting the body cured the pneumonia, and the last center on the list took healthy lungs for transplantation.".
Why can doctors refuse organs? For example, says Vasyl Strilka, a 20-year-old boy is waiting for a heart transplant. He is not in the first emergency status, and his expected life expectancy is at least a few more months.
And the donor who appeared in the system and is suitable for him is 59 years old. According to the indicators, this heart could be suitable for a 20-year-old, but transplantologists will think about whether it is worth transplanting an old heart into a young one. Maybe it is better to wait for another one that will work longer.
Or maybe there's a 70-year-old man who's lower in the waiting list because of age, but a 59-year-old heart would be perfectly fine for him.
Or to put it another way: a 20-year-old guy is already in the first emergency status, the predicted life expectancy is a week. That is, he will either die or receive a 59-year-old heart. In this case, doctors will transplant him, let the heart live not for 15 years and then there will be a retransplantation, but for four or five. And for the guy this is not only a chance to live these years, but also a chance for a retransplantation.
Are there any possible abuses by doctors here? When patients higher on the list are not called, but are noted as having refused, being sick, abroad, etc., the organ is then given "by arrangement." Vasyl Strelka replies that the patient may indeed not be called, he may have contraindications right now, he may refuse transplantation right now:
"In any case, such cases are recorded on paper with the signature of the responsible person, which makes it possible to understand. The final selection of the recipient is based on the results of an immunological compatibility test, these results are also documented.".
Can doctors, transplant coordinators, somehow enter data into the system so that specific centers receive certain organs? Doctors suggested in conversations that supposedly problems are likely at the human factor stage before entering data into the UHIST. Because technically, all the interlocutors have no questions about the UHIST, and they praised the automated system.
As an example, one interlocutor cited Germany, where cases of such conspiracies were allegedly proven. When a patient's clinical data was changed so that he became an emergency just before the desired donor organ appeared in the system. Conventionally, the transplant center changes the data in the system so that their patient acquired emergency status, and then the transplant coordinator enters the donor's data - and the system automatically combines them.
“If this happened in Germany, then theoretically it could happen here too,” says Strelka. “But by formalizing relations and taking into account cooperation between the transplant center and the procurement base, we reduce the likelihood of such things. Because the transplant center understands that the organ will most likely come to them anyway, according to the contract. This reduces the incentive to somehow play around. For four years, we had fewer emergency statuses and they were written out more streamlined. Therefore, in 2021, we wrote out the criteria for emergency statuses. For example, a patient in the first cardiac status must already be on ECMO.” When the heart and lungs are supported artificially, the person is still alive.
How high quality are organ transplants in Ukraine?
Some doctors pointed out that supposedly weaker teams can perform transplants because their management has become tense and signed contracts, while centers with stronger specialized teams for a particular organ practically do not operate.
“This is a complex story,” Vasyl Strilka answers. “The first (after a 15-year break) heart transplant in Ukraine took place in the Kovel District Hospital. Did it ever perform transplants? No. Was there anyone to do it? No. The head, Oleg Samchuk, wanted to — and they did everything they could. They launched brain death diagnostics there.
When a donor appeared there, they invited Boris Todurov (who once performed the first heart transplant in Ukraine) to perform the transplant. The team was already standing next to him and learning, including Roman Domashych, who is already performing heart transplants in Lviv. Then the time came when they realized that they could do it themselves.
"There are not only Boris Todurov, but up to a dozen cardiac surgeons who have performed heart transplants at least once. This is how we are doing professional demonopolization, increasing the pool of those who are able to do it, and a person can have a choice.".
We need three to five centers that can transplant a specific organ in order not to be dependent on one particular leader, adds Vasyl Strilka. There are already six liver transplantation teams: "Feofania", two teams at the Shalimov Institute, Okhmatdyt, Lviv Territorial Medical Association, "Oberih".
"If the head of the institution is interested in transplantation, he will lure good transplantologists to work - on a quarter or half-time basis.".
When there are several people who are potentially suitable for a particular organ, the system checks which of them has been in the queue the longest, who has given consent during their lifetime to have their organs removed in the event of their death.
The state pays well for transplantation. This allows us not to take money from the patient. When we calculated the tariff, we told the transplantation centers: calculate it so that you never have to take money from the patients.
So that you can pay a normal salary to the team. And at the same time, the state saves a million hryvnias on each kidney transplant compared to what we used to pay Belarusians (under the treatment abroad program). We also save more than a million on heart transplants. In addition, transplantation raises the level of the entire hospital. Then it needs to raise its laboratory, cardiologists, anesthesiologists.
I ask about the Kyiv case, which the doctors told off the record. When they sent a team of transplantologists to the States for training, they trained them, they brought them back — and they don't transplant. Vasyl Strelka says that the team was sent to the US because there was a problem — no one had transplanted lungs in Ukraine.
The first lung transplant in Lviv was performed when Polish doctors arrived and performed it together with local doctors. The Lviv residents had already performed the second one themselves. But one of the team went to work in Poland.

Later, Vasyl Strilka met a cardiac surgeon, a transplantologist of Ukrainian origin, Serhiy Melnychuk, who works at Mass General Hospital. This is a world-class hospital. One of the clinical bases of Harvard Medical School. Melnychuk helped her agree to teach lung transplants to 13 doctors from Ukraine. The core of the team — 11 doctors — were from Feofania, two more cardiac surgeons — from other institutions.
The Christian Medical Association helped with accommodation and logistics. The team spent three months there. They trained and upon their return, they independently performed several lung transplants in Ukraine.
But again, the bottleneck of the Ukrainian system, says Strelka. Transplanting lungs is more difficult than a heart, kidney, or liver. After all, the lungs have contact with the external environment. And if there is some kind of infection in the hospital that performs the transplant, then against the background of immunosuppression (suppression of the immune system, which is artificially given to the patient so that the body does not reject the transplanted organ), this infection progresses and the person has a high risk of dying.
"For the lungs to be suitable for transplantation, the donor must be from a very good intensive care unit," explains Vasyl. "From one where they treat very well. Then there is a higher probability that in the event of a diagnosis of brain death, the patient will have lungs suitable for transplantation. Very few hospitals can treat patients who either recover or are brain dead and have suitable lungs in this way. Lviv residents were able to perform lung transplantation because their intensive care unit is well-organized.".
"Feofania" is now receiving many victims of hostilities, and this also takes up the resources of the teams and equipment. Therefore, the question is not about trained doctors, says Strelka, but about several factors: "Because you can transplant lungs, but in the next ward there will be a patient with some kind of resistant microflora (i.e., a hospital infection, where there will be bacteria that antibiotics do not work on) and because of immunosuppression, the person will not survive.".
In various hospitals, it is precisely because of hospital-acquired infections that people who receive transplants sometimes do not survive. The spread of such serious infections that are resistant to antibiotics was previously spoken about by First Deputy Minister of Health Serhiy Dubrov.
And here we come to the last important issue of the system - the survival rate of Ukrainians after transplants.
Several doctors said off-record that teams that are better at transplanting and have higher survival rates transplant fewer organs compared to hospitals that have contracts and transplant more organs.
In their opinion, this is unfair even to the patient, who should be operated on by the best specialists and who should know in which hospital the risks of survival or death are higher. There are no publicly available statistics.
“Not yet. Someday,” Strelka replies. He says that survival figures will not be made public for now:
"On average, our indicators are a little worse than the European average. If we look at hospitals that performed three or four transplants on seriously ill patients due to emergency status, and two of them died, you can't evaluate the system here. In order to publish statistics, you need to show a breakdown by each center.
If one center performed three transplants on three critically ill patients, and one died, the survival rate would be 67%. Is that good or bad? And someone who performed 100 transplants would have a survival rate of 90%. And then no one would go to the center where there were three patients.
But they have 67% not because their hands are crooked, but because there are not yet adequate figures for assessment.
There is another side to the coin.
Can we take any measures against centers with worse survival rates? Some countries publish such rates. And there, seriously ill patients have almost no chance of a transplant. Because no one wants to take them, because they will spoil the statistics.
Because a seriously ill patient has a 70% chance of dying and not surviving after transplantation. And they play football with him.
We are only in the early stages: if we do this, the centers will not accept patients who could survive. Internally, we show the data to the centers, but publicly at this time it will be more of a detriment to the transplant system. The words that some people have worse results and more transplants, and some people have fewer and better results, are not supported by anything. We see that in centers that do more transplants, the results are better.
This is due to several factors:
– they gain experience; even if someone was very smart but did two transplants, and someone worked hard and did 40, I would go to the one who did 40. The best heart transplant outcome is now at the Heart Institute. Everyone from their last 21 transplants is alive;
– we still need more transplant teams; if they say that a doctor is great, most likely he is. And then either his administration starts working according to the existing rules, or he changes the hospital. If we say that we trust only these two teams and send everyone there, then we will never meet the need for transplants in Ukraine.”.

